 
As a result, the committee has recommended that the Oxford-AstraZeneca vaccine’s benefits outweigh its risks, with tremendous potential for preventing infections and deaths from SARS-CoV-2 infection 14. WHO Global Advisory Committee on Vaccine Safety has concluded that the available data do not suggest an overall increase in clotting conditions following the administration of the Oxford-AstraZeneca vaccine. The Oxford–AstraZeneca vaccine was temporarily paused in several European countries due to reports of thromboembolic events in vaccinated individuals 13. Most side effects of the Oxford–AstraZeneca vaccine are mild, including injection site pain, fatigue, headache, muscle pain, feeling or being sick, fever, or chills 1 or 2 days after vaccination. Unsolicited adverse events include lymphadenopathy and Bell’s palsy 12. Reported serious adverse events included acute myocardial infarction and cerebrovascular lesions, as thrombosis. Systemic responses included vomiting, diarrhea, fatigue, headache, muscle pain, chills, joint pain, and fever 8, 11. The three most frequent recorded immediate adverse events (within the first fifteen minutes) for COVID-19 vaccines included vagal response (30%), anxiety reaction (24%) and dizziness (21%) 10.Īccording to the Food and Drug Administration (FDA), the most common adverse events among participants in the Pfizer-BioNTech phase 3 clinical trials were short-term local responses including pain, redness and swelling at the injection site. On Aug 2021, 20,906, 174 (60.1%) of Saudi population were vaccinated with at least one dose of COVID-19 vaccine and 11,374,999 (32.0%) were fully vaccinated as documented by Saudi Ministry of Health (MOH) 9. After vaccination, the cells produce the spike protein, stimulating the immune system to attack the SARS-CoV-2 virus 8. It contains the genetic materials of the spike protein. 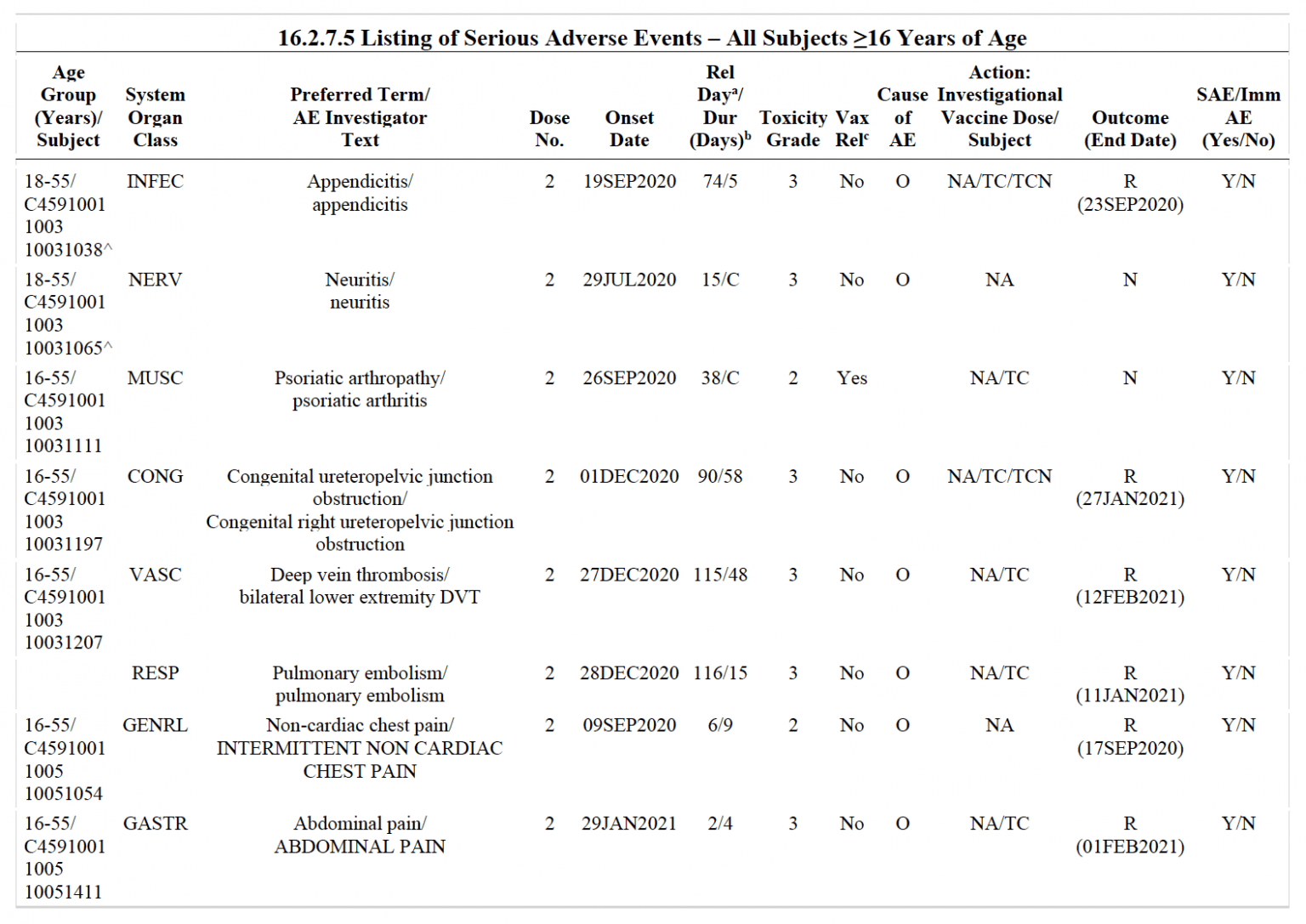
Oxford-AstraZeneca (AZD1222) vaccine is a replication-deficient chimpanzee viral vector based on a weakened version of a common cold virus (adenovirus) that causes infections in chimpanzees. Two doses of the vaccine produce high SARS-CoV-2 neutralizing antibody titers and robust antigen-specific CD8+ and Th1-type CD4+ T-cell responses 7. Pfizer-BioNTech COVID-19 (BNT162b2) vaccine is a lipid nanoparticle-formulated, nucleoside-modified mRNA vaccine encoding the prefusion spike glycoprotein of SARS-CoV-2. The most commonly approved and used vaccines in the kingdom of Saudi Arabia are Pfizer-BioNTech and Oxford-AstraZeneca (AZD1222) 6. 
Vaccines can reduce susceptibility among the uninfected and reduce the viral spread in those who are infected 5. Population-based vaccination is the best way to achieve herd immunity and prevent disease and community spread of infection 4. As of Sept 24, 2021, there were about 412 million confirmed cases of COVID-19, and about 5.8 deaths, reported to World Health Organization (WHO) worldwide 2, along with devastating medical, economic, and social consequences 3. Further cohort studies are recommended to investigate the long-term adverse events of COVID-19 vaccines.Ĭoronavirus disease 2019 (COVID-19) is an infectious disease caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) 1. Most of systemic and local adverse events were mild in nature. Adverse events were more frequent in females and younger age groups for both vaccines. No significant difference was recorded between both vaccines regarding overall systemic adverse events however, they were more frequent following the first dose of AstraZeneca vaccine compared to Pfizer-BioNTech vaccine, while the reverse was observed for the second dose. The most common reported systemic adverse events in both vaccines respectively were general fatigue (23.1% and 25.1%), fever (18.5% and 27.2%), myalgia (20.6% and 20.3%), and headache (15.2% and 17.2%). Recipients of Pfizer-BioNTech vaccine had a higher percentage of local adverse events (24.8% versus 9.8% in AstraZeneca vaccine). Immediate adverse events were reported by 1.04% and 2.09% for Pfizer-BioNTech and Oxford-AstraZeneca vaccines, respectively, with no serious events. A cross-sectional study was conducted among 958 individuals, 7 days after receiving either Pfizer-BioNTech or Oxford-AstraZeneca vaccines during June 2021. However, this study compares these adverse events between the two main COVID-19 vaccines used in Saudi Arabia (Pfizer-BioNTech and Oxford-AstraZeneca) using telemedicine technology. 
Previous studies investigated the frequency of different adverse events of COVID-19 vaccines. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
